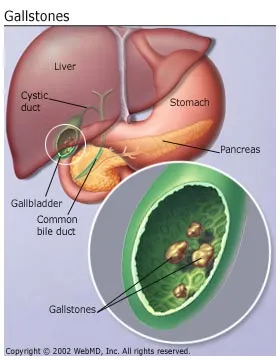
What Is Ovarian Cancer?
This cancer begins in the ovaries, the twin organs that produce a woman's eggs and the main source of the female hormones estrogen and progesterone. Treatments for ovarian cancer have become more effective in recent years, with the best results seen when the disease is found early.
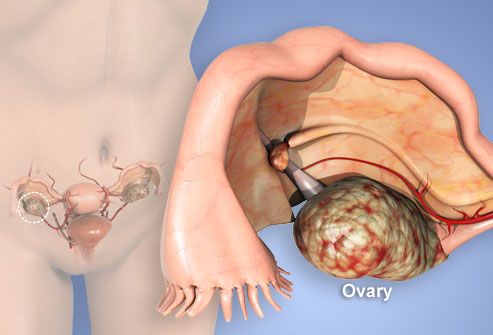
Symptoms
Symptoms include:
- Bloating or pressure in the belly
- Pain in the abdomen or pelvis
- Feeling full too quickly during meals
- Urinating more frequently
These symptoms can be caused by many conditions that are not cancer. If they occur daily for more than a few weeks, report them to your health care professional.
Risk Factor: Family History
A woman's odds of developing ovarian cancer are higher if a close relative has had cancer of the ovaries, breast, or colon. Researchers believe that inherited genetic changes account for 10% of ovarian cancers. This includes the BRCA1 and BRCA2 gene mutations, which are linked to breast cancer. Women with a strong family history should talk with a doctor to see whether closer medical follow-up could be helpful.
Risk Factor: Age
The strongest risk factor for ovarian cancer is age. It's most likely to develop after a woman goes through menopause. Using postmenopausal hormone therapy may increase the risk. The link seems strongest in women who take estrogen without progesterone for at least 5 to 10 years. Doctors are not certain whether taking a combination of estrogen and progesterone boosts the risk as well.
Risk Factor: Obesity
Obese women have a higher risk of getting ovarian cancer than other women. And the death rates for ovarian cancer are higher for obese women too, compared with non-obese women. The heaviest women appear to have the greatest risk.
Ovarian Cancer Screening Tests
There are two ways to screen for ovarian cancer before it causes symptoms or shows up during a routine gynecologic exam. One is a blood test for elevated levels of a protein called CA-125. The other is an ultrasound of the ovaries. Unfortunately, neither technique has been shown to save lives when used in women of average risk. For this reason, screening is only recommended for women with strong risk factors.
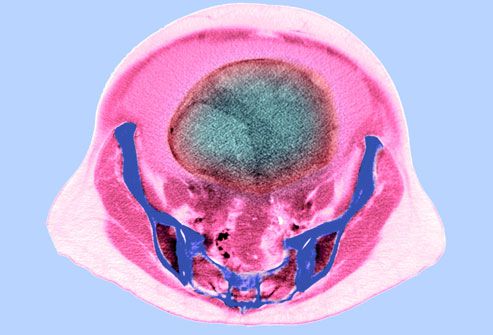
Diagnosing Ovarian Cancer
Imaging tests, such as ultrasound or CT scans (seen here), can help reveal an ovarian mass. But these scans can't determine whether the abnormality is cancer. If cancer is suspected, the next step is usually surgery to remove suspicious tissues. A sample is then sent to the lab for further examination. This is called a biopsy. Sometimes a sample taken with a needle can also be used for diagnosis.
Stages of Ovarian Cancer
The initial surgery for ovarian cancer also helps determine how far the cancer has spread, described by the following stages:
Stage I: Confined to one or both ovaries
Stage II: Spread to the uterus or other nearby organs
Stage III: Spread to the lymph nodes or abdominal lining
Stage IV: Spread to distant organs, such as the lungs or liver
Stage II: Spread to the uterus or other nearby organs
Stage III: Spread to the lymph nodes or abdominal lining
Stage IV: Spread to distant organs, such as the lungs or liver
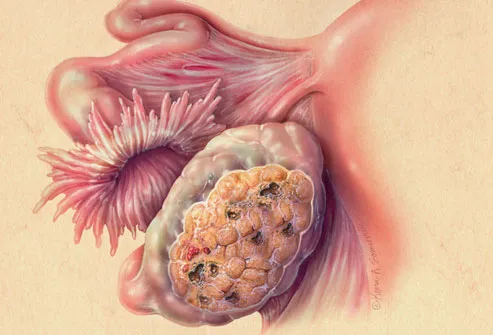
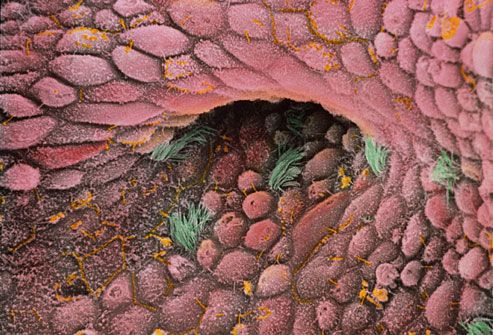
Types of Ovarian Cancer
The vast majority of ovarian cancers are epithelial ovarian carcinomas. These are malignant tumors that form from cells on the surface of the ovary. Some epithelial tumors are not clearly cancerous. These are known as tumors of low malignant potential (LMP). LMP tumors grow more slowly and are less dangerous than other forms of ovarian cancer.
Ovarian Cancer Survival Rates
Ovarian cancer can be a frightening diagnosis, with five-year relative survival rates that range from 89% to 18% for epithelial ovarian cancer, depending on the stage when the cancer was found. But keep in mind that these odds are based on women diagnosed from 1988 to 2001. The treatments and outlook may be better for people diagnosed today. For LMP tumors, the five-year relative survival rates range from 99% to 77%.
Ovarian Cancer Surgery
Surgery is used to diagnose ovarian cancer and determine its stage, but it is also the first phase of treatment. The goal is to remove as much of the cancer as possible. This may include a single ovary and nearby tissue in stage I. In more advanced stages, it may be necessary to remove both ovaries, along with the uterus and surrounding tissues.
Chemotherapy
In all stages of ovarian cancer, chemotherapy is usually given after surgery. This phase of treatment uses drugs to target and kill any remaining cancer in the body. The drugs may be given by mouth, through an IV, or directly into the belly (intraperitoneal chemotherapy.) Women with LMP tumors usually don't need chemo unless the tumors grow back after surgery.
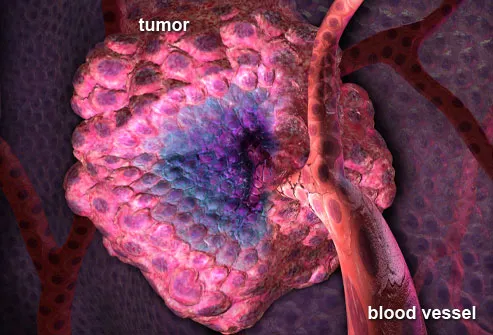
rgeted Therapies
Researchers are working on therapies that target the way ovarian cancer grows. A process called angiogenesis involves the formation of new blood vessels to feed tumors. A drug called Avastin blocks this process, causing tumors to shrink or stop growing (seen in the illustration here). Avastin is approved for other cancers, but ovarian cancer researchers are still testing this therapy, which can have serious side effects.
After Treatment: Early Menopause
When women have both ovaries removed, they can no longer produce their own estrogen. This triggers menopause, no matter how young the patient. The drop in hormone levels can also raise the risk for certain medical conditions, including osteoporosis. It's vital that women have regular follow-up care after being treated for ovarian cancer.